BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
URL: http://ijmm.ir/article-1-1617-en.html
2- Department of Microbiology, School of Medicine, Kermanshah University of Medical Sciences, Kermanshah, Iran
3- Behbahan Faculty of Medical Sciences, Behbahan, Iran
4- Department of Virology, School of Medicine, Hamadan University of Medical Sciences, Hamadan, Iran ,
Cockroaches, which are extensively colonized in humans and hospitals, may act as the vectors of antibiotic-resistant bacteria (1, 2). They are tropical, but most species live in warm conditions (3). Cockroaches live close to humans and in poor sanitation (4, 5) and play a role as mechanical vectors that mechanically transmit pathogens (6, 7). However, in some studies, these species are also introduced as biological vectors (7, 8). Cockroaches can indirectly transmit microorganisms and other disease causative agents by contaminating food (9) and causing intestinal or foodborne diseases (3, 10). The Blattella germanica (German cockroach), with a light yellowish-brown color and a length range of 1-2.5 cm (11-13), is the most abundantly distributed cockroach species. In hospitals, cockroaches might serve as potential carriers in the epidemiology of nosocomial infections, especially the transmission of drug-resistant Escherichia coli, Pseudomonas aeruginosa, Klebsiella spp., and several other potential pathogens (5, 14). Recently, one of the important concerns in healthcare systems is the resistance of Enterobacterales to carbapenems because of the increasing mortality and morbidity in hospitalized patients (15, 16). Carbapenems are the last-line treatment of Enterobacterales infections, making resistance to these agents a major challenge for clinicians (15, 17). This study aimed to determine antibiotic susceptibility and resistance genes to carbapenems in E. coli isolates from Blattella germanica by dot-blot assay in Hamadan hospitals in west Iran.
Sampling and Bacterial Isolation
In this cross-sectional study performed during April 2018-September 2018, 109 Blattella germanica were randomly collected from different hospitals in Hamadan, Iran, using hand catch sticky traps and sterile gloves. The collected cockroaches were immediately transferred to the Microbiology Laboratory of Hamadan University of Medical Sciences, Iran, in clean, sterile plastic bags (18). Only whole and alive cockroaches were evaluated in this study. The Blatella germanica were identified by a specialist based on reliable taxonomic keys in the Department of Entomology, Insectarium, Hamadan University of Medical Sciences (19). The tubes containing Blatella germanica were filled with 70% ethanol for 5 min to disinfect the outer surfaces and were then allowed to air dry. Next, Blatella germanica samples were washed with normal saline to remove excess ethanol. Finally, their gut was dissected with sterile forceps under a microscope, and the instruments were sterilized after each dissection. E. coli isolates were identified and confirmed by conventional microbiological and biochemical tests (20, 21). In brief, 500 μL of peptone solution was inoculated in nutrient agar and blood agar plates. The inoculated plates were then incubated aerobically at 37°C for 24 h (22).
Antibiotic Susceptibility Testing
The antibiotics disks (Mast Group Co, UK) of gentamicin (GM, 10 µg), ciprofloxacin (CIP, 5 µg), ampicillin (AMP, 10 µg), imipenem (IMI, 10 µg), meropenem (MEN, 10 µg), ertapenem (ERT, 10 µg), and cefotaxime (CTX, 30 µg) were used. According to the Clinical and Laboratory Standard Institute (CLSI 2018) guidelines, the antibiotic susceptibility test was completed through the disk diffusion method. For quality control and the evaluation of results, E. coli ATCC25922 was used as a positive control.
Identification of Carbapenemases Genes by Dot-Blot Assay
In this study, DNA Flow Technology) Master Diagnostica, Spain (provided the platform for rapid analyses in the membrane-based reverse dot-blot hybridization process. DNA target molecules were directed to complementary capture probes immobilized in the matrix pores. The reaction between the target DNA and probes in a three-dimensional environment result in high signal intensity in a brief period. There are three distinct regions in this kit, identified as B: hybridization control, CI: exogenous amplification control, BG: endogenous amplification control (ß-globin human fragment) using the position of the points created around the points. In the present study, the dot-blot assay was utilized to identify antimicrobial resistance in the E. coli isolated from Blatella germanica (www.masterdiagnostica.com).
In this study, out of 109 Blatella germanica taken from the Intensive Care Units of different hospitals in Hamadan, 31 E. coli cases were isolated. The pattern of antibiotic resistance was resistance to ampicillin in 31 isolates (100%), cefotaxime in seven isolates (22.58%), cotrimoxazole in 14 isolates (41.94%), ciprofloxacin in 14 isolates (41.94%), imipenem in two isolates (6.45%), ertapenem in three isolates (4.46%), meropenem in three isolates (6.46%), and gentamicin in nine isolates (29.03%) (Figure 1).
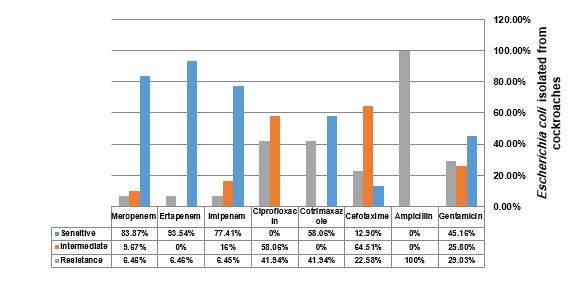
Figure 1. Antibiotic resistance pattern of Escherichia coli isolated from Blatella germanica.
The results obtained from the dot-blot assay showed that out of 31 E. coli isolated from Blatella germanica, four isolates (12.90%) that carried bla NDM had the highest frequency among E. coli isolates (Figure 2). However, only one isolate (3.22%) with bla OXA-48 gene was detected in this study. Other genes, including IMI, GES, VIM, GIM, SPM, SIM, IMP, OXA23, 24, 51 and OXA 58, KPC, SME, NMC were not detected.

Figure 2. Detection of bla NDM and bla OXA-48 genes by dot blot assay.
Cockroaches in sensitive locations, such as hospitals, are more harmful than in other areas due to the unique conditions and particular hospitalized individuals and can impact environmental, human, and community health (23, 24). This study aimed to find carbapenem resistance genes in E. coli isolated from Blatella germanica using the dot-blot assay at Hamadan Hospitals, Iran. The evaluation of the antimicrobial susceptibility pattern showed that E. coli strains isolated from cockroaches had the highest antibiotic resistance to ampicillin (100%), cotrimoxazole (41.94%), ciprofloxacin (41.94%), and gentamicin (29.03%). On the other hand, the lowest resistance was to imipenem (6.45), ertapenem (6.46), and meropenem (6.46%).
Many studies have been conducted in this field. For example, in agreement with our results, Wannigama et al. stated that the frequency of resistance to ampicillin, imipenem, and gentamicin, was 100%, 0%, and 28.2%, respectively (25). Pignato et al. reported the highest resistance rates against ampicillin (22.71%), tetracycline (19.41%), sulfamethoxazole (16.84%), and streptomycin (14.28%) (26). However, this frequency may be different in some studies; for example, Moges et al. assessed Blatella germanica as a source of highly pathogenic bacteria and reported different results from the pattern in our study (27). Several antibiotic resistance patterns of pathogenic bacterial strains have been reported in Blatella germanica in Bangladesh, India, and Nigeria (5, 23, 28). The high level of resistance to ampicillin in E. coli can be attributed to the overuse of this antibiotic. This variation in prevalence may result from diverse factors, such as different antiseptics and their concentrations in hospitals.
The results obtained from the abundance of beta-lactamase genes and resistance to broad-spectrum beta-lactam antibiotics showed that the New Delhi metallo-β-lactamase (bla NDM) gene had the highest frequency (12.9%) in E. coli isolates. The bla OXA-48 gene was next in terms of prevalence and frequency (3.033%). In line with these findings, Hosseinzadeh et al. investigated the antibiotic susceptibility pattern of Klebsiella pneumoniae isolates and determined the frequency of carbapenemase-producing K. pneumonia. These authors stated that bla NDM and bla OXA-48 genes were detected in 27 (10.9%) and 2 (0.9%) isolates, respectively (29). In other investigations, Nobari et al. discovered three bla NDM-positive isolates among 42 carbapenem-resistant K. pneumoniae isolates (19, 30). Moreover, Fazeli et al. revealed six bla NDM-positive isolates among 49 carbapenem-resistant K. pneumoniae isolates (31). In recent years, bla NDM has been found in some neighboring nations of Iran. The most frequent carbapenemases found in the Persian Gulf Cooperation Council (i.e., Saudi Arabia, United Arab Emirates, Oman, Kuwait, Qatar, and Bahrain) were bla OXA-48 (35 isolates) and bla NDM (16 isolates) (32, 33). Therefore, one overarching theme from prior research and our findings is the rising prevalence of bla NDM in hospitals, which causes concern. Considering these results, we recommend limiting carbapenem prescriptions and implementing effective infection control policies to avoid the spread of resistant strains.
The proliferation of carbapenem-resistant isolates has been a growing concern in recent years. Because these antibiotics are used as the last line of medicine to treat infections caused by gram-negative bacilli, including members of the Enterobacterales family, carbapenem-resistant isolates carrying bla NDM were nearly resistant to all antibiotics tested; resistance to this gene may grow in the near future, posing a significant health risk. As a result of the increasing frequency of bla NDM found in our study, we propose limiting carbapenem prescriptions and implementing efficient infection control policies to avoid the spread of resistant strains. Finally, because cockroaches play a crucial role in spreading Enterobacterales and multidrug-resistant (MDR) strains, effective prevention and control strategies are required to reduce vector-borne diseases.
We want to thank all members of the microbiology and Entomology laboratory of Hamadan University of Medical Sciences.
The authors fund this article.
Conflicts of Interest
There is no conflict of interest between the authors.
Received: 2022/01/7 | Accepted: 2022/03/15 | ePublished: 2022/05/25
| Rights and permissions | |
 |
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. |








