BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
URL: http://ijmm.ir/article-1-2237-en.html


 , Mohamad Reza Nazer2
, Mohamad Reza Nazer2 

 , Seyed Mahmoudreza Hashemi Rafsanjani3
, Seyed Mahmoudreza Hashemi Rafsanjani3 

 , Majid Nouri1
, Majid Nouri1 

 , Saeed Soleiman-Meigooni4
, Saeed Soleiman-Meigooni4 


2- Department of Infectious Diseases and Tropical Medicine, School of Medicine, Isfahan University of Medical Sciences, Isfahan, Iran
3- Department of General Medicine, Faculty of Medicine, Aja university of Medical Sciences, Tehran, Iran
4- Infectious Diseases and Tropical Medicine Research Center (IDTMRC), Aja university of Medical Sciences, Tehran, Iran ,
Brucellosis, a zoonotic disease impacting both animals and humans, poses significant economic and public health challenges globally. Brucella melitensis and Brucella abortus are the primary culprits behind epidemic brucellosis (1, 2). Additionally, human brucellosis can stem from various Brucella species, including B. canis and B. suis, often transmitted through infected animal organs or the consumption of unpasteurized dairy products. This disease notably contributes to economic losses due to reduced milk production and livestock abortion. Despite therapeutic efforts, brucellosis treatment has not yielded absolute success, with instances of disease relapses documented. Moreover, widespread and inappropriate antibiotic use has raised concerns about antibiotic resistance in Brucella isolates (3-6).
It is now firmly established that Brucella is an intracellular bacterium capable of evading macrophage defenses. Furthermore, it induces significant mitochondrial fragmentation within 48 hours of entering various cell types. Consequently, effective antibiotics for brucellosis treatment must possess the ability to penetrate macrophages and eliminate the bacteria. However, in many clinical laboratories, routine antibiotic susceptibility testing is not feasible due to the absence of biosafety level 3 facilities (7-9). Consequently, there is limited available data regarding the antibiotic susceptibility of Brucella species, making it imperative to investigate. Thus, this study aimed to assess the antibiotic susceptibility profile of Brucella spp. isolated from humans in a systematic review and meta-analysis.
This systematic review and meta-analysis study was conducted based on the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guideline 2020 (1).
Search Strategy
Two authors performed a systematic search of literature in the following electronic databases: PubMed, Web of Science, and Scopus. No time limitation was defined and all English studies from the beginning until September 2023 were included. The relevant medical subject heading (MeSH) terms and related keywords were used in combination to build the search strategy; (“brucella” OR “brucellosis” OR “brucel*”) AND (“antibiotic” OR “susceptibility” OR “resistance” OR “sensitivity” OR “sensitive” OR “resistant”).
Eligibility Criteria
Our eligibility criteria were defined based on the PICO framework: (P) Population: patients with brucellosis. (I) antibiogram test. (C) susceptibility or resistance. (O) Not applicable. Those studies that did not include human samples, did not report outcomes, or performed any antibiogram tests were excluded. Studies that were not in English, were also excluded.
Data Extraction and Outcome Measures
A standardized Excel sheet was prepared for data extraction. Two independent authors performed the data extraction. Disagreement between these two authors was discussed and resolved by a third author. The data extraction sheet included the following study characteristics: first author’s name, year of publication, country, total number of samples, susceptible and resistant samples for trimethoprim, rifampicin, doxycycline, tetracycline, ciprofloxacin, gentamicin, and streptomycin.
Data Synthesis and Statistical Analysis
The pooled susceptibility/resistance ratios were calculated using the random effects model and Mantel-Haenszel method along with the 95% confidence intervals. For assessing the heterogeneity of the included studies, the I2 (I square) test was used. The Mantel-Haenszel method and random effects model were used for pooling the effect sizes. For testing the overall significance of the random model, a z-test was performed Potential publication bias was graphically assessed by creating funnel plots for each of the aforementioned groups. R (R Foundation for Statistical Computing, Vienna, Austria) and RStudio (RStudio, Inc., Boston, MA) were used for the statistical analysis and creation of forest and funnel plots.
Our initial search retrieved 931 articles from PubMed, Scopus, and Web of Science, from which 185 duplicates were removed. After screening the title and abstract of 746 records, 66 full texts were retrieved, among which 15 studies (Figure 1) were included based on our eligibility criteria (4, 5, 10-22). More detail regarding the study characteristics of the included studies is summarised in Table 1.
Based on the pooled susceptibility ratios, among the 630 samples of Brucella spp., 98% (95% CI: 85% - 100%) were susceptible to trimethoprim. Further information regarding the susceptibility of Brucella spp. against trimethoprim is available in Figure 2. The pooled resistance ratio of Brucella spp. against trimethoprim is available in Appendix 1.
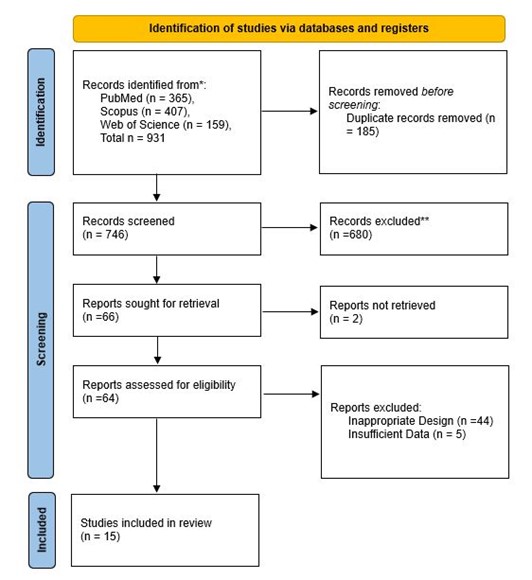
Figure 1. PRISMA flowchart of the included studies
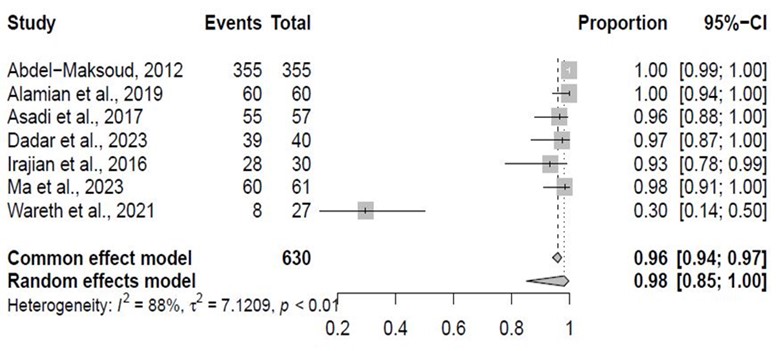
Figure 2. The pooled susceptibility ratio of Brucella spp. against trimethoprim
Based on the pooled susceptibility ratios, among the 1255 samples of Brucella spp., 82% (95% CI: 54% - 95%) were susceptible to rifampicin. Further information regarding the susceptibility of Brucella spp. against rifampicin is available in Figure 3. The pooled resistance ratio of Brucella spp. against rifampicin is available in Appendix 2.
Based on the pooled susceptibility ratios, among the 1344 samples of Brucella spp., 100% (95% CI: 78% - 100%) were susceptible to doxycycline. Further information regarding the susceptibility of Brucella spp. against doxycycline is available in Figure 4. The pooled resistance ratio of Brucella spp. against doxycycline is available in Appendix 3.

Figure 3. The pooled susceptibility ratio of Brucella spp. against rifampicin
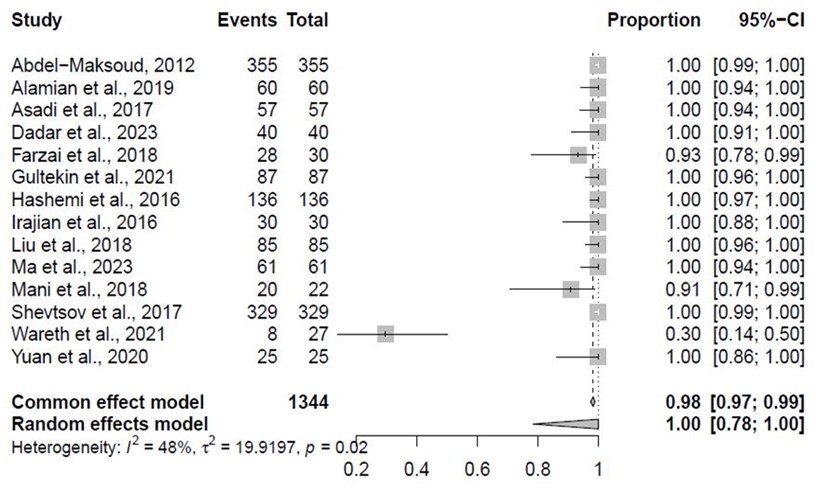
Figure 4. The pooled susceptibility ratio of Brucella spp. against doxycycline
Based on the pooled susceptibility ratios, among the 942 samples of Brucella spp., 100% (95% CI: 85% - 100%) were susceptible to tetracycline. Further information regarding the susceptibility of Brucella spp. against tetracycline is available in Figure 5. The pooled resistance ratio of Brucella spp. against tetracycline is available in Appendix 4.
Based on the pooled susceptibility ratios, among the 893 samples of Brucella spp., 100% (95% CI: 82% - 100%) were susceptible to ciprofloxacin. Further information regarding the susceptibility of Brucella spp. against ciprofloxacin is available in Figure 6. The pooled resistance ratio of Brucella spp. against ciprofloxacin is available in Appendix 5.

Figure 5. The pooled susceptibility ratio of Brucella spp. against tetracycline
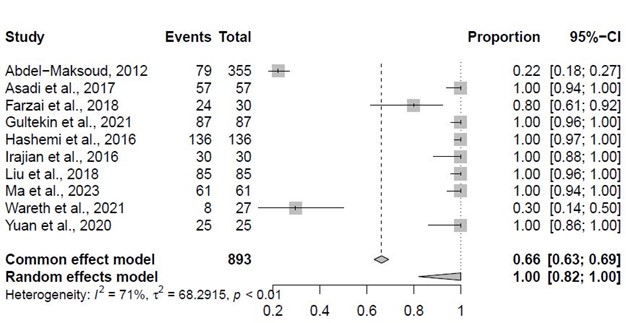
Figure 6. The pooled susceptibility ratio of Brucella spp. against ciprofloxacin
Based on the pooled susceptibility ratios, among the 906 samples of Brucella spp., 97% (95% CI: 96% - 98%) were susceptible to gentamicin. Further information regarding the susceptibility of Brucella spp. against gentamicin is available in Figure 7. The pooled resistance ratio of Brucella spp. against gentamicin is available in Appendix 6.
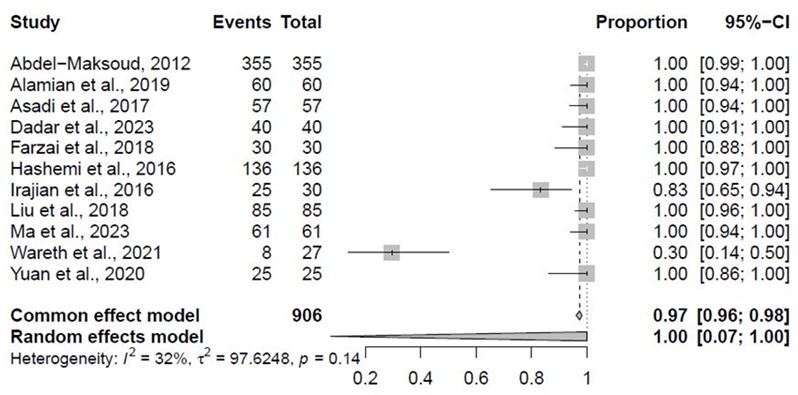
Figure 7. The pooled susceptibility ratio of Brucella spp. against gentamicin
In our systematic review and meta-analysis study, we evaluated the susceptibility of Brucella spp. to various antibiotics. The results demonstrated varying levels of susceptibility among these samples, indicating that certain antibiotics, such as trimethoprim, doxycycline, tetracycline, ciprofloxacin, and gentamicin, were effective against Brucella spp. infections. However, susceptibility to rifampicin was lower in comparison. These findings provide insights into potential treatment options for Brucella infections, supporting the importance of antibiotic selection in managing this disease.
Brucellosis primarily affects individuals who come into contact with farm animals, particularly cattle, sheep, and goats. Additionally, cases have been reported in those who consume raw milk, driven by traditional beliefs in its health benefits. Diagnosis typically relies on serological tests for antibodies or isolating the Brucella bacterium (10, 23, 24). However, the gold standard involves isolating the causative agent, which requires high-level biosafety laboratories due to the organism's high infectivity. Consequently, limited efforts are made to isolate and identify Brucella spp. from clinical samples, leading to potential misidentifications (11, 25-27).
Similarly, Lopez-Merino et al. found that cotrimoxazole and rifampin exhibited limited inhibitory activity against Brucella strains. In an endemic region for human brucellosis in Turkey, B. melitensis isolates demonstrated the highest resistance rate to cotrimoxazole (46.3%), while resistance to rifampin was observed in only 9.7%. In many developing countries, inappropriate antibiotic use is the primary driver of antibiotic resistance, resulting in the annual consumption of a multitude of antibiotics (28-31). Furthermore, Iran has reported significantly higher usage of systemic antibacterial agents like broad-spectrum penicillin, third-generation cephalosporins, and quinolones compared to other countries. It is known to exert an in vitro inhibitory effect against Brucella spp. due to its efficient intracellular diffusion. In our study, 98.5% (59/60) of the tested Brucella isolates with MIC≤1 μg/mL were classified as sensitive to rifampin based on the CLSI breakpoints for slow-growing bacteria. However, one Brucella strain exhibited resistance to rifampin with a MIC of 1.5 μg/mL. Notably, a high rate of rifampin resistance has been previously documented in Egyptian field strains (64%), as well as in Brazil (36.73%), Turkey (9.7%), and Malaysia (70%) (13, 32-35).
It's important to take into account that a significant portion of individuals with brucellosis cannot endure extended rifampin therapy due to its adverse gastrointestinal effects. Consequently, the concurrent use of streptomycin and doxycycline has been identified as the preferred treatment regimen, followed by the combination of rifampin and doxycycline, as there have been no reported treatment failures or relapses with these regimens. Nevertheless, several studies have cautioned against the indiscriminate use of rifampin due to the increased occurrence of intermediate sensitivity to these drugs (15, 36-39).
The World Health Organization has provided treatment recommendations for adults with acute brucellosis, endorsing a six-week regimen that combines doxycycline with either rifampicin or streptomycin. These guidelines remain applicable today. Nonetheless, there have been reports indicating that cases of brucellosis accompanied by osteoarticular and visceral complications are less prone to relapse when treated with a triple therapy approach involving streptomycin, rifampicin, and doxycycline (17, 40-44). Furthermore, an extensive review and meta-analysis of 30 randomized controlled trials have suggested that the preferred treatment should include combinations like doxycycline with gentamicin or triple regimens (e.g., doxycycline, rifampicin, and gentamicin). Despite combination therapy, there have been reports of relapse rates as high as 10%. Importantly, these relapses were primarily attributed to inadequate treatment due to issues such as incorrect dosing or poor patient compliance, rather than antimicrobial resistance. As a result, antimicrobial susceptibility testing is currently not considered indispensable in the management of brucellosis cases. Also, doxycycline has become the preferred tetracycline derivative for Brucella infection treatment due to its favorable pharmacokinetics (45-49).
In our systematic review and meta-analysis, we assessed the susceptibility of Brucella spp. to different antibiotics. Our findings revealed varying degrees of susceptibility among these samples. Notably, trimethoprim, doxycycline, tetracycline, ciprofloxacin, and gentamicin exhibited effectiveness against Brucella spp. infections. In contrast, rifampicin showed lower susceptibility. These results offer valuable insights into potential antibiotic choices for treating Brucella infections, emphasizing the significance of antibiotic selection in the management of this disease.
Not applicable.
Conflicts of Interest
The authors declare that they don’t have any conflict of interest.
None .
Received: 2023/10/7 | Accepted: 2024/01/9 | ePublished: 2024/01/29
| Rights and permissions | |
 |
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. |





